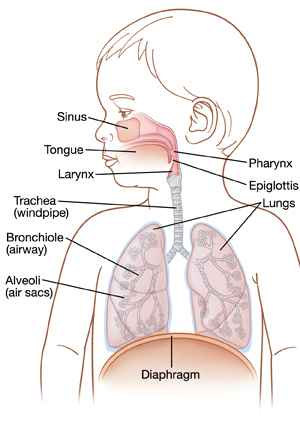
Bronchiolitis is an infection involving the lower respiratory tract(Lungs and the tubes inside them) and occurs mainly in young babies between 2 to 6 months old.
Fig: Anatomy of the Human Breathing(Respiratory) System
How do they present?
Usually they present with
- Breathing difficulties
- Cough
- reduced feeding
- Irritability
- Wheezing(Musical noise from the chest)
- In very young babies they may present with apnea(stopping of breathing).
It is cause by viral infection of the bronchioles(small tubes carrying air inside the Lungs). Respiratory syncytial virus (RSV) is the most common pathogen, causing 50-90% of cases. In addition to RSV other viruses like Rhinovirus, Influenza, enterovirus etc can also cause bronchiolitis. This condition involves excessive production of mucus, cell debris and swelling which cause narrowing and obstruction of small airways.
Is there any seasonal variation?
The Peak season for bronchiolitis is during winter and rainy months, but can occur in other periods as well and more common in Urban than rural areas.By their first birthday most children would have had this infection in varying severity.
What are the risk factors for bronchiolitis?
The usual environmental risk factors are
- Viral infection in siblings(Brothers and sisters) or family members
- Nursery/playgroup attendance
- Passive smoking
- Overcrowding
Other risk factors include
- Preterm birth (<37 weeks) and
- Breathing problems at birth
- Low birth weight(<2.5 kg)
- Age less than 12 weeks
- Other medical conditions which weakens the child(eg heart defects)
Breast-feeding is considered protective and mothers must try to give be encouraged for this and other reasons.
How do these children present?
Early symptoms are similar to that of a viral infection with runny nose, cough and fever. Nearly half of them get better and the rest get worse with cough, breathing difficulties, poor feeding, Cyanosis(blue around the lips due to lack of oxygen), and very rarely apneas(stopping of breathing).
Please contact your doctor if symptoms aren’t improving and worsens with any of the above. In a typical child Bronchiolitis gets worse by day 3-4 before they get better.
How to we diagnose Bronchiolitis and are there any tests?
The diagnosis is mainly clinical based on the symptoms and after examining the child.Some investigations include
- Pulse oximeter- To check the oxygen content in the blood
- Nasopharyngeal aspirate to check for viruses
- Chest X Ray
- Complete Blood count
- Electrolytes and Kidney function tests
- Blood and urine culture: If high temperature
- Arterial blood gases
Not all these tests are needed for every child and must be prioritised depending on the condition of the child
How do we treat bronchiolitis as an outpatient
Most of these babies can be treated as an outpatient and don’t need hospital admission. The key aim should be to maintain adequate fluid intake, nutrition, temperature control and maintain oxygenation. In most of the times the symptoms last for 2 weeks and in some children upto 4 weeks. Some children might get worse and therefore please get your child assessed by your doctor regularly.
Please Consult with your doctor urgently in case of
- Poor feeding (<50% usual intake over the previous 24 hours)
- Lethargy
- History of apnoea
- Fast breathing >70 breaths/minute
- chest wall recession
- Cyanosis- Blueness around the lips and other body parts
- and if you are worried about your child
Some of these children will need hospital admission to administer Fluids, Oxygen, IV antibiotics, and ventilation in Intensive care.
What is the outlook?
In general most of these children make a full recovery from bronchiolitis. In hospitalised children the recovery may be very slow in some instances and close observation is essential.
Can we prevent or minimise the disease severity
yes to some extent by the following measures
Vaccines:
Flu vaccines are available but can be given only after 6 months.Vaccine for RSV(RSV immunoglobulin (RSV-Ig))is available but very expensive in the Indian market presently and not affordable for many
In addition to vaccines the spread of the virus can be controlled by proper hand washing and minimising the contact with the infected child.
Author: Dr.S.Boopathi MD, DNB, MRCPCh(UK)
![]()